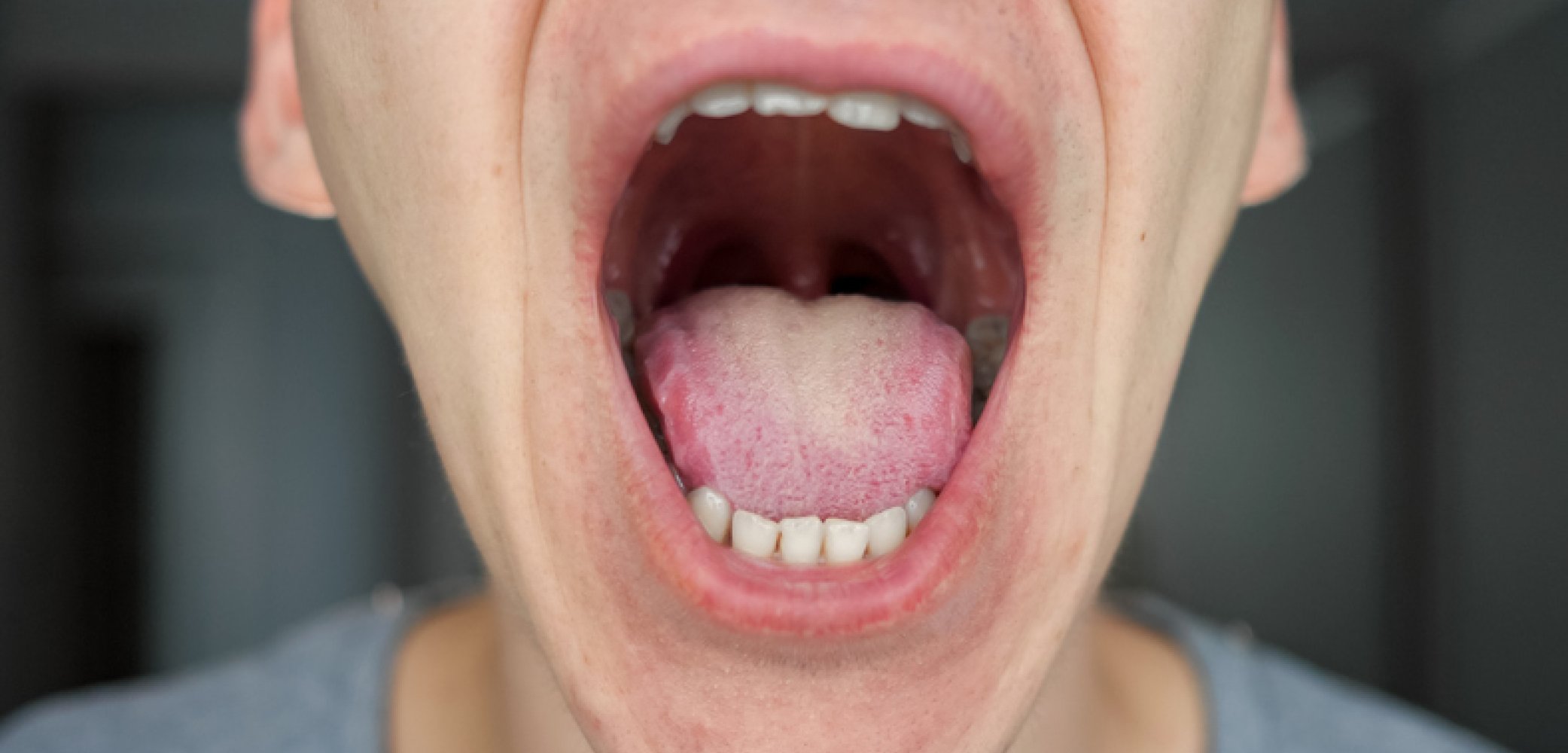
A mouth biopsy becomes important when small but persistent changes raise questions that cannot be answered through a standard clinical exam, and this simple procedure helps clarify what those changes might mean. Oral specialists often explain that biopsies offer a clear picture when visual evaluation alone cannot provide certainty, and this clarity allows both patients and clinicians to move forward with confidence. According to our editor’s research, many professionals use biopsies not as a last step but as an early tool to prevent delays in care, and this practical approach reduces unnecessary worries. You might find yourself wondering why a harmless-looking spot draws attention, and that curiosity is exactly why understanding the basic signs makes a real difference. Some patients express concern about discomfort, yet specialists emphasize that the procedure is brief and generally well tolerated.
How do persistent sores signal deeper concerns?
Persistent sores attract attention when they remain unchanged for weeks, and this simple timeline often acts as the earliest sign that something needs closer evaluation. A sore that heals slowly or keeps returning may indicate irritation, infection, or other underlying processes, and recognizing these patterns helps guide the decision to perform a biopsy. Dentists often highlight that most oral sores are harmless, yet the few that persist beyond normal healing time should not be ignored because they offer valuable diagnostic clues. As a result of our editor’s reviews, many reports show that patients delay care thinking the sore will improve, and this delay sometimes makes evaluation more complicated. Paying attention to duration, sensitivity, and changes in texture provides helpful context when discussing concerns with a specialist. You might feel tempted to wait for improvement, but patterns that linger beyond expected limits deserve careful attention.
Why do unusual color changes raise suspicion?
Unusual color changes in the mouth often prompt further evaluation, and these changes may appear red, white, or even mixed in tone. Specialists suggest that patches with striking contrast compared to surrounding tissues deserve a closer look because color shifts sometimes reflect changes in cell behavior. According to our editor’s research, clinicians commonly observe that white patches called leukoplakia or red patches known as erythroplakia can occasionally carry a risk that requires clarification through biopsy. These areas may feel normal or slightly rough, and their presence alone does not confirm a significant problem, yet persistent or expanding patches often justify additional investigation. People sometimes assume color changes are related to brushing or eating habits, but consistency over time distinguishes temporary irritation from something more meaningful. Understanding your normal oral appearance helps you notice differences quickly and describe them accurately during your appointment.
What role do lumps or thickened areas play?
Lumps or thickened spots inside the mouth often act as early indicators that tissue structure has changed, and these differences encourage clinicians to consider a biopsy. These areas might appear on the tongue, gums, cheeks, or the floor of the mouth, and their texture can vary from firm to slightly rubbery. As a result of our editor’s reviews, many dental professionals explain that not all lumps are concerning, yet persistent or growing areas offer essential diagnostic information. Some lumps form due to irritation, biting, or minor trauma, and these typically resolve on their own, but growth over time differentiates ordinary swelling from lesions needing evaluation. You may feel unsure about what qualifies as “growth,” and paying attention to subtle size changes helps guide the conversation. Specialists rely on these observations because structural differences sometimes reveal conditions that are invisible during routine checks.
How do unexplained bleeding or tenderness contribute to evaluation?
Unexplained bleeding inside the mouth can indicate fragile tissues, and when this bleeding occurs without brushing or irritation, it may encourage a closer look. Tenderness that develops in one specific area, especially without a known injury, can also serve as a sign that tissues require additional evaluation. Dentists often mention that minimal bleeding is common during brushing for some people, yet isolated bleeding spots or persistent tenderness raise different questions. According to our editor’s research, many clinicians consider bleeding that continues for more than a few days as a valid reason to investigate further. People sometimes attribute tenderness to new food, stress, or minor habits, and while these factors play a role, tenderness that does not improve becomes more meaningful. A biopsy helps determine whether the tissues are responding normally or showing patterns that need attention.
Why do numb areas or strange sensations matter?
Numbness or tingling inside the mouth can appear unexpectedly, and these sensory changes often prompt a more thorough evaluation. Specialists explain that nerves in the oral cavity respond to pressure, inflammation, or structural shifts, and changes in sensation might indicate that something requires closer analysis. As a result of our editor’s reviews, dentists emphasize that numb areas lasting more than a few days should not be overlooked because sensation patterns offer valuable diagnostic clues. Many people ignore tingling or chalk it up to biting the cheek, yet persistent or spreading numbness provides a reason for concern. Sensory symptoms help clinicians determine whether a biopsy is appropriate, especially when combined with visible tissue changes. Understanding the normal sensations inside your mouth helps you identify differences early and describe them accurately.
How do non-healing extraction sites guide decisions?
After a tooth extraction, the area typically heals in a predictable timeframe, and delays in this process might signal the need for a biopsy. Specialists describe that the tissues should slowly fill and strengthen within weeks, and any deviation from this pattern deserves attention. According to our editor’s research, dental professionals often observe that chronic inflammation or unusual tissue growth around an extraction site becomes a common reason for biopsy. You might assume that healing varies widely, and while there are differences, significant delays or unusual changes should not be ignored. Some patients experience discomfort and believe it is part of normal recovery, but persistent symptoms add important context. A biopsy in these situations helps clarify whether the healing process is occurring as expected.
What do changes in chewing or swallowing indicate?
Changes that affect chewing or swallowing sometimes arise from small lesions or growths, and these functional differences may guide specialists toward performing a biopsy. You may notice difficulty moving the tongue smoothly or experience discomfort when food touches a specific area, and these subtle changes provide helpful clues. As a result of our editor’s reviews, many clinicians mention that swallowing discomfort paired with visible tissue changes increases the likelihood of recommending a biopsy. People often attribute these issues to temporary irritation or stress, yet persistent difficulties deserve attention. These functional symptoms do not always relate to severe conditions, but they create a clearer picture when combined with visual or sensory signs. Observing how your mouth feels during daily meals offers simple yet important feedback.
How does a family or personal history influence evaluation?
A family or personal history of oral conditions sometimes increases the importance of taking small symptoms seriously, and this background information often shapes the decision to recommend a biopsy. Specialists highlight that genetics can influence how tissues respond to irritation or environmental factors, and this context helps determine which signs carry more weight. According to our editor’s research, clinicians frequently adjust their level of concern depending on the patient’s history because early evaluation reduces uncertainty. Many patients hesitate to share detailed background information, yet doing so allows your provider to interpret symptoms accurately. This approach does not imply that history alone determines outcomes, but it helps prioritize when a biopsy becomes helpful. Understanding your family patterns may encourage you to monitor small changes more closely.
Why does duration remain one of the strongest indicators?
Duration often becomes the most straightforward indicator because tissues inside the mouth heal quickly under normal conditions, and delays stand out as meaningful clues. Dentists explain that two-week timelines offer a simple reference point when evaluating persistent lesions or discomfort. As a result of our editor’s reviews, many specialists feel confident recommending evaluation when symptoms exceed normal healing patterns because this proactive approach prevents unnecessary uncertainty. People sometimes wait for symptoms to fade, assuming they are minor, yet waiting may complicate diagnosis. Monitoring how long changes remain helps guide decisions and provides clarity during your appointment. Duration remains an easy and reliable measure that anyone can track at home.