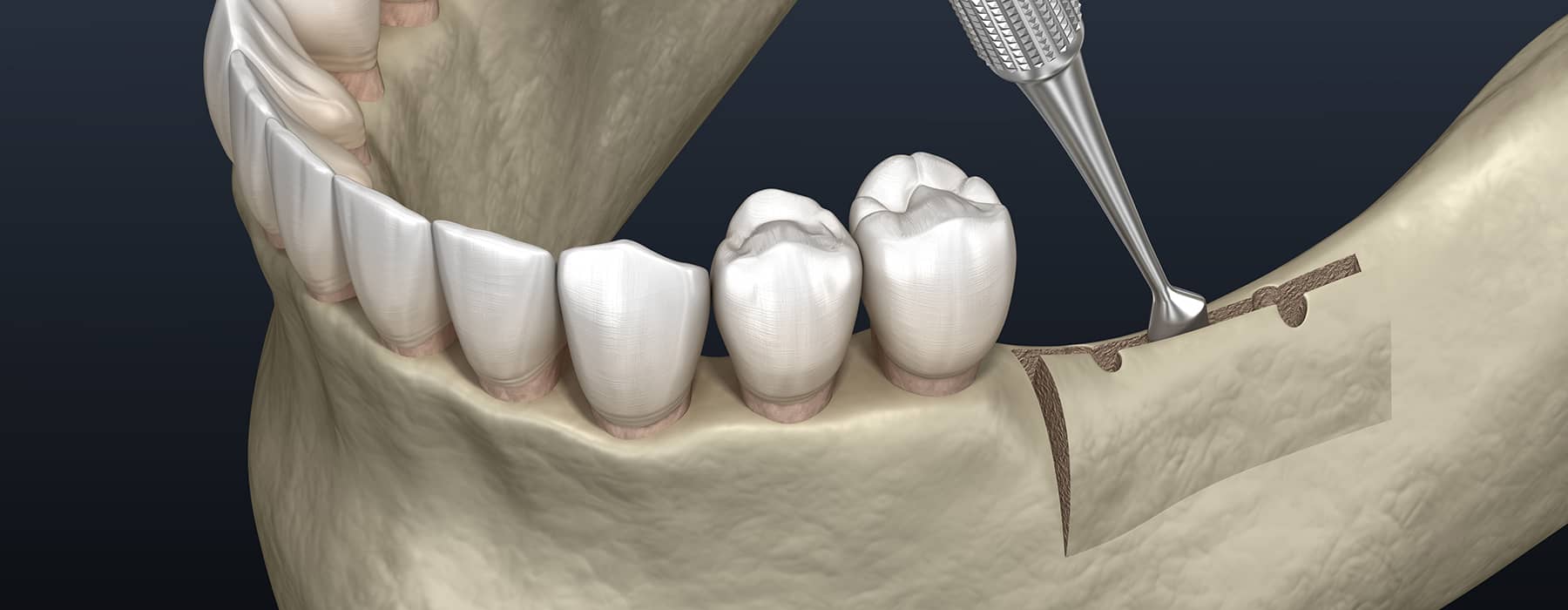
Alveoloplasty reshapes uneven jawbone so dentures, implants, or surgical closures seat comfortably, lowering sore spots, improving stability, and helping gums heal after extractions.
What does alveoloplasty involve?
Alveoloplasty is surgical smoothing of the alveolar ridge. The goal is a rounded, comfortable foundation for future restorations. Surgeons remove sharp edges and bony ledges carefully. The gum is lifted, bone contoured, and the gum closed. Stitches support healing and protect the reshaped ridge. The result feels smoother to the tongue and cheeks. Later prosthetics sit more evenly on the prepared surface.
When is alveoloplasty recommended?
Dentists consider it before dentures that require stable support. It helps when a ridge is thin or irregular. It is common after multiple extractions in one area. It prepares sites for tissue borne and implant borne options. It eases chronic denture sore spots that never settle. It can free a trapped cheek under a sharp spur. Your clinician weighs benefits against tissue preservation goals.
How does it differ from socket preservation?
Socket preservation protects volume with grafts after extraction. It seeks height and width for future implants. Alveoloplasty removes small irregularities to improve contour. The first builds; the second refines and smooths. Sometimes both appear in a single treatment plan. A graft may set, then edges get polished. The sequence depends on anatomy and final goals.
Who performs the procedure safely?
Oral and maxillofacial surgeons commonly lead this work. Periodontists perform ridge shaping around soft tissue needs. Experienced general dentists may handle smaller cases responsibly. The choice depends on complexity and adjacent structures. Nerve proximity raises the need for advanced training. Sinus floor closeness also increases planning demands. Your referral reflects anatomy, not just convenience.
What happens during the appointment?
Local anesthesia numbs the gums and underlying bone. A small incision allows precise visualization and access. The surgeon uses burs and rongeurs to contour bone. Irrigation cools the site and clears debris continuously. Edges are checked with a gloved fingertip for smoothness. The gum is re positioned and sutured without tension. A gauze pack follows for gentle compression.
Will I need imaging beforehand?
Most plans start with recent dental radiographs for context. Panoramic views outline roots and overall ridge shape. Cone beam scans help when nerves are nearby. They also assist with implant oriented planning steps. Imaging supports safer flap design and instrument choices. Your clinician explains why each image truly matters. Good pictures shorten surgery and reduce surprises.
How is pain managed afterward?
Numbing medicine lingers for several comfortable hours. Many patients do well with over the counter options. Cold compresses help with swelling during the first day. Sleeping with the head elevated reduces throbbing sensations. Soft foods decrease pressure on tender tissues. Short walks support circulation and overall comfort. Most discomfort fades steadily within several days.
How long does healing take?
Initial gum closure occurs within one to two weeks. Sutures usually leave on schedule without issues. Bone reshapes more slowly beneath the surface. Early bone stability improves by six to eight weeks. Final remodeling continues for several months quietly. Your timetable depends on overall health and habits. The site should feel steadily easier each week.
What are the realistic risks?
Bleeding can continue if instructions are ignored. Bruising can appear on the cheek and jawline. Infection is uncommon with good oral hygiene. Nerve irritation is rare but deserves careful planning. Over reduction can lessen future denture stability. Under reduction can leave persistent sharp areas. Balanced contouring minimizes both of these outcomes.
Are there alternatives in some cases?
Selective tooth extraction can sometimes improve ridge shape. Targeted soft lining in a denture cushions hot spots. Minor enamel adjustments change bite stress distribution. Tissue conditioning improves inflamed denture bearing gums. Grafting may build areas rather than reduce them. Observation is reasonable when symptoms are minimal. Your plan should fit goals and timelines.
According to our editor’s research, what helps planning most?
According to our editor’s research, three habits stand out. Pre impression mock ups reveal pressure points before surgery. Marking sore spots on old dentures guides bone refinement. Bite records identify tilting that creates repeat injuries. Clear notes shorten chair time and recheck visits. Simple documentation often prevents avoidable revisions. Good photographs further improve team communication.
As a result of our editor’s reviews, which tools matter?
As a result of our editor’s reviews, consistency wins. Finger sweeps catch micro ridges better than sight alone. Colored pencils mark remaining edges on the bone. A small straightedge checks for hidden ledges. Irrigation syringes support clean postoperative care. These low tech tools deliver reliable, repeatable results. High polish beating high speed alone remains true.
What about special situations like diabetes?
Stable blood sugar supports predictable healing responses. Infections rise when glucose control is poor. Preoperative checks reduce unnecessary risk for patients. Antibiotic decisions follow individual medical histories carefully. Gentle tissue handling protects slower microvascular healing. Appointment timing considers meals and medications thoughtfully. Your medical team should coordinate details in advance.
What should denture wearers expect afterward?
New dentures rarely go in immediately without planning. Temporary liners can protect healing ridges as needed. Old dentures might be modified to sit lighter. Frequent follow ups remove high spots quickly. Expect several adjustments as swelling changes shape. Sore areas should improve within short intervals. Good fit usually requires patient feedback and patience.
How is alveoloplasty used before implants?
Implant supported plans often prefer preserved volume. Alveoloplasty then focuses on small edge smoothing. It also adjusts ridge width to match prosthetic planning. Surgeons protect critical bone near future implant paths. The objective remains a broad, healthy platform. Slight contour changes can improve implant emergence profile. Each alteration supports hygiene and long term maintenance.
How do surgeons decide timing?
Immediate contouring happens during large extraction visits. Delayed contouring follows bone growth and graft integration. Early work decreases later chair time for prosthetics. Delayed work respects fragile tissues after complex procedures. Both options aim for a stable, smooth ridge. The plan reflects anatomy, schedules, and comfort. Your clinician explains which path best suits you.
How can you prepare at home?
Stock soft foods like yogurt, soups, and eggs. Prepare cold packs and small towels in advance. Arrange a ride if sedation will be used. Set up a clean pillowcase for the first night. Place gauze and an irrigation syringe nearby. Fill recommended medications before the appointment time. A calm home supports a comfortable first day.
How to care for the site afterward?
Do not disturb the clot in the first hours. Avoid vigorous rinsing during the first day. Begin gentle salt water rinses when advised. Brush nearby teeth with care and patience. Keep fingers and tongues away from the stitches. Eat cool, soft foods until tenderness fades. Return if swelling worsens rather than improves.
When should you call your clinician?
Call for heavy bleeding that does not stop. Call for fever or spreading facial redness. Call for numbness that persists beyond expected windows. Call for sharp edges that cut the tongue. Call for bad taste with increasing swelling. Call if stitches loosen before advised removal. Prompt calls prevent small problems from growing.
How does alveoloplasty fit everyday timelines?
Most people return to work the next day. Heavy exercise waits until your clinician approves. Speaking and swallowing feel normal quickly. Diet expands as soreness continues to fade. Prosthetic steps resume on the planned calendar. Each check confirms progress and comfort improvements. The process should feel organized and predictable.
What does it feel like months later?
The ridge feels smoother to the tongue and cheeks. Chewing pressure spreads more evenly across tissues. Dentures or implants feel more stable day to day. Less rubbing means less inflammation and ulceration. Speech clarity improves when edges stop catching. Cleaning routines become simpler and more reliable. Confidence returns as discomfort recedes from memory.
How do teams avoid over contouring?
Measurements track original widths before bony changes. Wax ups reflect final tooth positions and forces. Surgeons favor minimal removal near thin walls. Communication with the lab shapes conservative plans. Trial bases reveal support before permanent steps. Rehearsal reduces surprises during final delivery. Less removal preserves future options and strength.
Will alveoloplasty change facial appearance?
Small contouring rarely affects facial fullness. Large reductions can slightly alter soft tissue support. Your clinician discusses any visible changes beforehand. Photographs can help set shared expectations early. Denture design also influences lip and cheek support. Balanced plans consider bone and prosthetic roles together. The overall goal favors function and comfort first.
What if you smoke or vape?
Nicotine reduces blood flow within healing tissues. The risk of complications rises with continued use. Stopping even briefly improves surgical outcomes markedly. Your team can suggest support options for quitting. Protecting the clot becomes easier without irritants. Gums heal faster and with less inflammation. Every smoke free day supports better results.
Why do follow up visits matter?
Healing looks different inside than it feels. Professionals look for specific early warning signs. Small adjustments now prevent large ones later. Suture removal should match the planned schedule. Denture relines may follow natural remodeling phases. Documentation ensures continuity across the full team. Consistent reviews protect your investment in health.
What costs should you expect?
Fees reflect time, imaging, and treatment scope. Additional grafting increases overall expense where needed. Sedation choices also influence budget decisions. Insurance coverage varies widely by region and plan. Pre authorizations help avoid unwelcome surprises later. Clear estimates encourage stress free preparation steps. Ask questions until the plan feels transparent.